What Are the Causes of Ulcerative Colitis?
While the exact cause of ulcerative colitis remains unclear, research indicates that a combination of genetics, environmental factors, and an overactive immune system significantly contributes to the development of this chronic condition in adults. If you’re experiencing persistent digestive issues, it’s crucial to seek care from a skilled specialist like Dr. Nilesh Mehta, MD, at Digestive Disease Care. With his expertise in gastroenterology, Dr. Mehta and his dedicated team provide personalized, state-of-the-art treatment plans aimed at achieving long-term remission and helping you regain your quality of life. For more information, contact us today or schedule an appointment online. We are conveniently located at 1991 Marcus Ave Suite M200, Lake Success, NY 11042.
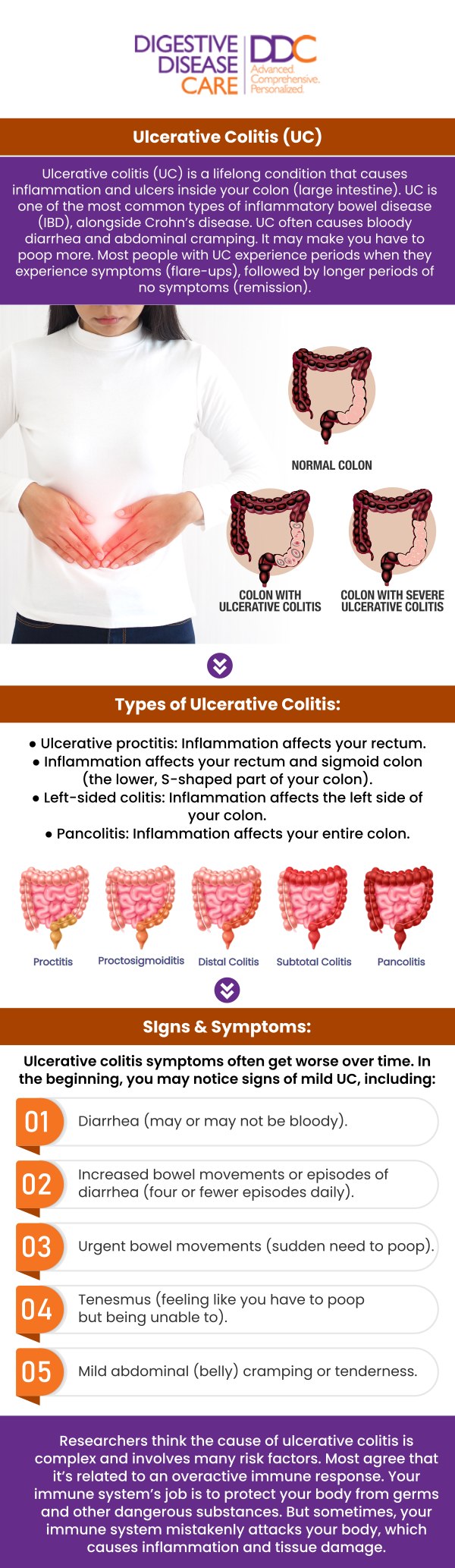
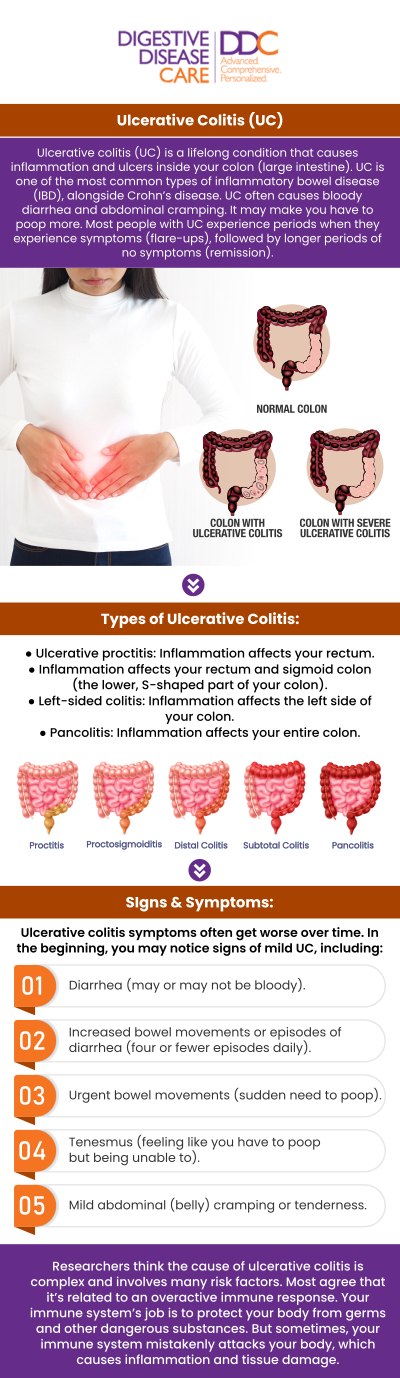
Table of Contents:
What causes ulcerative colitis?
How does genetics affect the development of ulcerative colitis?
What are the different types of ulcerative colitis?
Can ulcerative colitis lead to other health problems?
How Dr. Nilesh Mehta, MD and the Digestive Disease Care Team Help You Understand Ulcerative Colitis Causes in Lake Success, NY
Ulcerative colitis is a chronic inflammatory condition that affects the lining of the large intestine (colon) and rectum. It belongs to a group of diseases known as inflammatory bowel disease (IBD). Unlike occasional digestive upset, ulcerative colitis represents a persistent and abnormal inflammatory response that can disrupt normal digestion and lead to ongoing symptoms.
Although the precise cause remains unknown, researchers point to a combination of factors that contribute to the development of ulcerative colitis. The immune system plays a central role: when functioning correctly, the immune system defends the body from infection. In ulcerative colitis, the immune system mistakenly attacks healthy tissue in the colon, leading to inflammation and ulcers.
Key contributors to ulcerative colitis include:
• Immune system dysfunction: An overactive immune response targeting the gut lining.
• Environmental triggers: Certain lifestyle factors, diet, infections, or changes in gut flora may provoke inflammation.
• Genetic predisposition: Family history increases the likelihood of developing the disease.
• Microbiome imbalances: Alterations in the gut bacterial composition may influence immune reactions.
Inflammation from ulcerative colitis typically begins in the rectum and extends upward through the colon. The severity and extent of inflammation vary between individuals. Some people experience mild irritation, while others develop widespread inflammation that interferes with nutrient absorption and overall gastrointestinal function.
Because the causes are complex and multifactorial, managing ulcerative colitis often requires a tailored treatment plan focusing on reducing inflammation, maintaining remission, and improving quality of life.
Genetics plays a significant role in determining who may be more likely to develop ulcerative colitis. While ulcerative colitis does not follow a simple pattern of inheritance like some genetic diseases, certain gene variations have been linked to higher susceptibility.
Studies show that individuals with a family history of ulcerative colitis or other forms of inflammatory bowel disease are more likely to develop the condition themselves. This suggests that inherited genetic factors influence how the immune system functions and how the gut responds to environmental influences.
Important genetic insights include:
• Family risk: Relatives of people with ulcerative colitis are at a higher risk, indicating inherited predisposition.
• Gene variants: Specific genes related to immune regulation, barrier function, and inflammation have been associated with the disease.
• Shared genetic pathways: Some genetic markers are common to both ulcerative colitis and other autoimmune conditions.
• Complex inheritance: Multiple genes, rather than a single gene mutation, contribute to risk, along with environmental interactions.
It’s essential to understand that having a genetic predisposition does not guarantee someone will develop ulcerative colitis, but it increases the likelihood, especially when combined with triggers such as stress, infection, or changes in gut bacteria.
Genetic research continues to provide valuable insights that help clinicians understand disease mechanisms and potential future therapies targeting specific immune pathways.
Ulcerative colitis is classified based on how much of the colon is affected. These classifications help guide treatment decisions and determine the potential for complications.
Major types of ulcerative colitis include:
Ulcerative proctitis:
• Inflammation is limited to the rectum.
• Symptoms can include rectal bleeding and urgency.
• Often considered the mildest form.
Left‑sided colitis:
• Affects the rectum and lower portion of the colon up to the splenic flexure (left side of the abdomen).
• Symptoms may include abdominal cramping and bloody diarrhea.
Pancolitis:
• Inflammation affects the entire colon.
• Generally associated with more severe symptoms and greater risk of complications.
Distal colitis:
• Involves inflammation of the rectum and left colon.
• Symptoms may be similar to left‑sided colitis but with less extensive involvement.
Each type of ulcerative colitis carries a unique symptom profile and influences treatment strategy. Distinguishing which areas of the colon are inflamed helps your specialist personalize care, optimize medication management, and monitor for complications such as strictures or nutrient deficiencies.
Yes—ulcerative colitis can extend beyond the colon and lead to additional health issues if not properly managed. Chronic inflammation in the gut may affect other organ systems or create complications within the gastrointestinal tract.
Potential health problems linked to ulcerative colitis include:
• Severe bleeding: Chronic inflammation can cause ulcers that bleed, potentially leading to anemia.
• Dehydration and electrolyte imbalance: Frequent diarrhea can disrupt normal fluid and electrolyte balance.
• Increased colorectal cancer risk: Long‑standing ulcerative colitis, especially pancolitis, increases the lifetime risk of colorectal cancer.
• Strictures: Chronic inflammation can cause scarring that narrows the colon, leading to blockages.
• Growth problems (in adults): Persistent inflammation and poor nutrient absorption can affect weight and muscle mass.
• Extraintestinal manifestations: Joint pain, skin conditions, and liver inflammation can occur due to immune system dysregulation.
The likelihood and severity of these complications often correlate with disease duration, extent of inflammation, and how well the condition is controlled with medical therapy. Regular follow‑ups with a specialist, adherence to treatment plans, and appropriate screenings are vital to reducing risks and preserving long‑term health.
Living with or suspecting ulcerative colitis can be overwhelming—but patients in Lake Success, NY don’t have to navigate this journey alone. Dr. Nilesh Mehta, MD and the experienced team at Digestive Disease Care specialize in diagnosing, educating, and managing complex gastrointestinal conditions, including ulcerative colitis. Using a patient‑focused approach, they help individuals understand not just what the disease is, but why it may have occurred and how it can be controlled effectively.
Dr. Mehta brings deep expertise in gastroenterology with particular attention to inflammatory bowel diseases. This includes thorough clinical evaluations, advanced testing, and collaborative treatment planning. By identifying individual triggers—whether genetic factors, immune responses, or microbiome imbalances—Dr. Mehta ensures patients receive a customized plan that targets both symptoms and underlying contributors.
How the Digestive Disease Care team supports you:
• Comprehensive education about the causes and mechanisms of ulcerative colitis.
• Advanced diagnostic testing to evaluate inflammation, immune activity, and disease severity.
• Individualized treatment plans tailored to disease type (proctitis, left‑sided colitis, pancolitis) and lifestyle needs.
• Ongoing monitoring and care coordination to keep inflammation controlled and prevent complications.
At our Lake Success location, patients benefit from an environment that combines clinical excellence with compassionate support. Whether you’re newly diagnosed or seeking better disease control, Dr. Mehta and his team provide the tools and care needed to face ulcerative colitis with confidence. Our commitment to long‑term health outcomes helps residents of Nassau County and surrounding communities manage symptoms, reduce flare‑ups, and live fuller lives. For more information, contact us today or schedule an appointment online. We are conveniently located at 1991 Marcus Ave Suite M200, Lake Success, NY 11042. We serve patients from Lake Success, NY, Queens, NY, Hempstead NY, Roslyn NY, Jericho NY, Westbury NY, and surrounding areas.

Check Out Our 5 Star Reviews


Additional Services You May Like

Additional Services You May Like
- Abdominal Pain
- Acid Reflux
- Barretts Esophagus
- Bloating
- Capsule Endoscopy
- Celiac Disease
- Colon Cancer Screening
- Colonoscopy
- Constipation
- Crohns Disease
- Diarrhea
- Diverticulitis
- Esophageal PH Monitoring
- Fatty Liver
- Fibroscan
- Gallstones
- Gastroenterologist
- Gastric Chest Pain
- Gluten Intolerance
- Hemorrhoid
- Hemorrhoid Banding
- Hepatitis
- Irritable Bowel Syndrome
- Lactose Intolerance
- Pancreatitis
- Polyps
- Rectal Bleeding
- Stomach
- Ulcerative Colitis
- GI Urgent Care





