Complications of Pancreatitis and How They Can Be Prevented
Pancreatitis can lead to complications such as infections, pseudocysts, chronic pain, and digestive issues if not properly managed. Early detection and treatment are important to prevent these outcomes. Lifestyle changes, dietary guidance, and timely medical care can help reduce risks. Dr. Preeti Mehta at Digestive Disease Care in Melville, NY, and her team of board-certified gastroenterologists provide thorough evaluation and care to support long-term pancreatic health. For more information, contact us today or book an appointment online. We are conveniently located at 150 Broadhollow Rd, Suite 120-B, Melville, NY 11747.
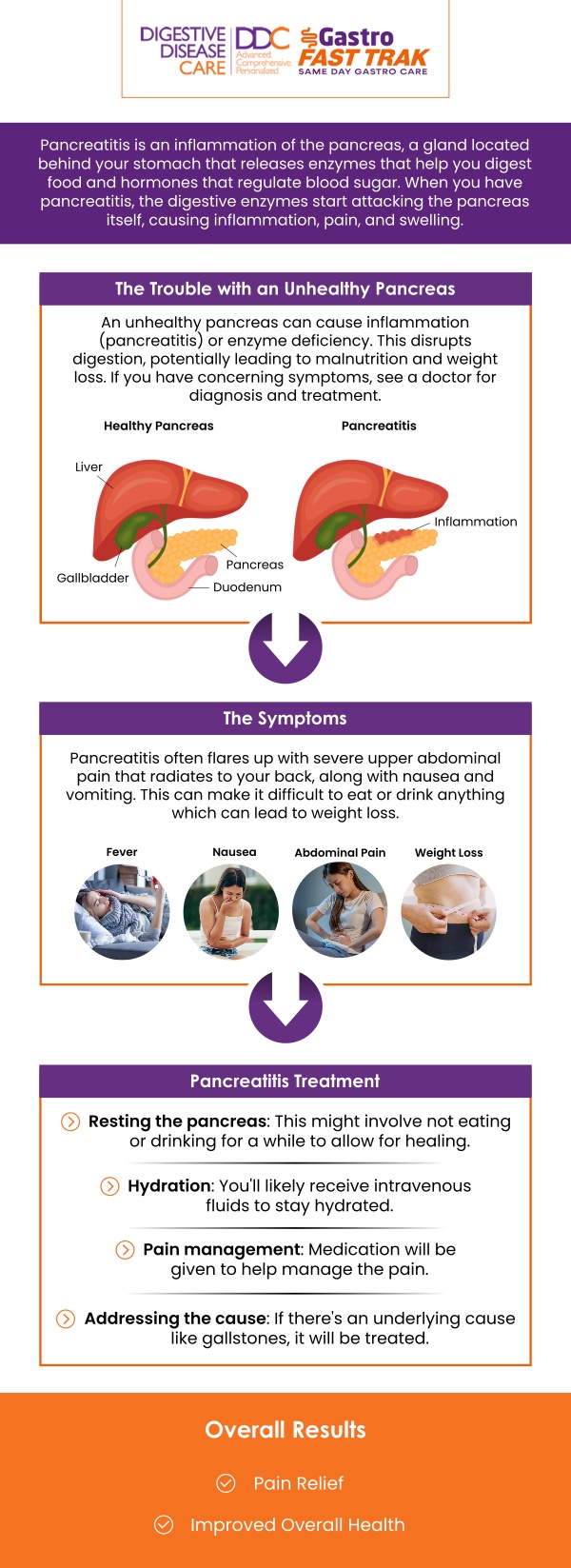
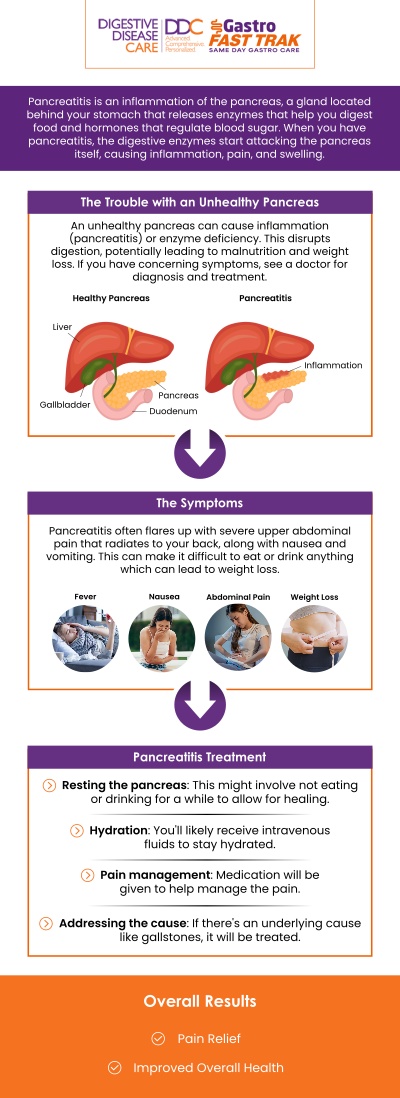
Table of Contents:
What are the common complications of pancreatitis?
What is the risk of developing an infection with pancreatitis?
Can pancreatitis cause chronic pancreatitis?
What is the link between pancreatitis and gallstones?
Pancreatitis Treatment You Can Trust: Dr. Preeti Mehta, MD at Digestive Disease Care
Pancreatitis, whether acute or chronic, can lead to a variety of complications that affect digestion and overall health. Understanding potential complications helps patients seek timely treatment and prevent severe outcomes.
• Pancreatic pseudocysts:
Fluid-filled sacs may form in or around the pancreas. These can cause pain, nausea, or infection if they grow large or rupture.
• Infections:
Inflamed pancreatic tissue can become infected, requiring antibiotics or sometimes surgical intervention.
• Digestive problems:
Pancreatitis may impair the production of digestive enzymes, leading to poor nutrient absorption, diarrhea, and weight loss.
• Diabetes:
Chronic inflammation can damage insulin-producing cells in the pancreas, increasing the risk of developing diabetes over time.
• Organ complications:
Severe pancreatitis can affect the lungs, kidneys, and heart, especially during acute episodes, sometimes leading to multi-organ dysfunction.
• Chronic pain:
Persistent inflammation or damage can lead to long-term abdominal pain, which may require ongoing management strategies.
• Scar tissue and fibrosis:
Repeated episodes of pancreatitis may result in scarring, which can interfere with pancreatic function.
Early recognition and management of pancreatitis can minimize the risk of these complications. Dr. Preeti Mehta, MD at Digestive Disease Care and her team of board-certified gastroenterologists provide evaluation and treatment to reduce complications and support long-term pancreatic health.
Infections are a serious concern in pancreatitis because inflamed pancreatic tissue is susceptible to bacterial invasion. Understanding the risk and recognizing early signs is crucial for timely treatment.
• Acute necrotizing pancreatitis:
In severe cases, areas of pancreatic tissue can die and become infected, requiring antibiotics or drainage procedures.
• Symptoms of infection:
Fever, chills, worsening abdominal pain, or increased heart rate may indicate infection in the pancreas.
• Timing:
Infections often occur several days into a severe episode of pancreatitis, making monitoring critical in patients.
• Preventive measures:
Prompt medical attention for pancreatitis, maintaining hydration, and controlling inflammation can reduce the likelihood of infection.
• Treatment strategies:
If infection develops, patients may require intravenous antibiotics and minimally invasive drainage to remove infected tissue.
Dr. Preeti Mehta at Digestive Disease Care in Melville, NY and her team of board-certified gastroenterologists provide careful monitoring and management of pancreatitis patients to detect and treat infections early, minimizing risk and supporting recovery.
Yes, repeated or severe episodes of pancreatitis can lead to chronic pancreatitis, a long-term condition that gradually impairs pancreatic function. Understanding this progression is important for prevention and management.
• Repeated inflammation:
Acute pancreatitis episodes can damage pancreatic tissue over time, leading to chronic inflammation.
• Permanent changes:
Chronic pancreatitis results in scarring and fibrosis, which may reduce the pancreas’s ability to produce digestive enzymes and insulin.
• Symptoms:
Persistent abdominal pain, weight loss, fatty stools, and digestive difficulties are common in chronic pancreatitis.
• Risk factors:
Heavy alcohol use, genetic predisposition, or gallstone-related pancreatitis increase the likelihood of developing chronic disease.
• Long-term management:
Lifestyle modifications, enzyme replacement, dietary changes, and monitoring of blood sugar levels help manage chronic pancreatitis and prevent complications.
Dr. Preeti Mehta at Digestive Disease Care in Melville, NY and her team of board-certified gastroenterologists provide personalized care to reduce the risk of chronic pancreatitis, manage symptoms, and maintain digestive and metabolic health.
Gallstones are one of the most common causes of pancreatitis, as they can block the pancreatic duct and trigger inflammation. Understanding this connection helps patients recognize risk factors and take preventive measures.
• Duct obstruction:
Gallstones may temporarily block the pancreatic duct, preventing digestive enzymes from flowing properly and causing inflammation.
• Acute attacks:
Blockage can result in sudden, severe abdominal pain, nausea, vomiting, and elevated pancreatic enzymes.
• Recurrent pancreatitis:
If gallstones continue to obstruct the duct, repeated pancreatitis episodes can occur, increasing the risk of chronic pancreatitis.
• Preventive measures:
Gallbladder removal or monitoring for gallstones in high-risk patients can prevent pancreatitis episodes.
• Treatment strategies:
Early diagnosis of gallstone-related pancreatitis allows timely interventions, including dietary adjustments and endoscopic procedures.
Dr. Preeti Mehta at Digestive Disease Care in Melville, NY and her team of board-certified gastroenterologists provide comprehensive care for patients with gallstone-related pancreatitis. Their approach focuses on preventing recurrences, managing inflammation, and supporting long-term pancreatic health.
Effective pancreatitis management requires evaluation, personalized care, and careful monitoring to prevent complications. Dr. Preeti Mehta and her team provide comprehensive treatment plans tailored to each patient.
• Personalized evaluation:
Careful review of symptoms, medical history, and risk factors ensures accurate assessment.
• Diagnostic testing:
Blood work, imaging, and other tests identify the severity and cause of pancreatitis.
• Targeted treatment plans:
Treatments may include dietary guidance, medications, hydration therapy, and procedural interventions if necessary.
• Ongoing monitoring:
Regular follow-ups prevent recurrence, detect complications early, and maintain pancreatic function.
• Patient education:
Patients learn lifestyle modifications and strategies to reduce flare-ups and support digestive health.
Dr. Preeti Mehta, MD at Digestive Disease Care and her team of board-certified gastroenterologists in Melville, NY provide compassionate, patient-focused care. They help patients manage pancreatitis effectively, reduce complications, and maintain long-term digestive wellness. For more information, contact us today or book an appointment online. We are conveniently located at 150 Broadhollow Rd, Suite 120-B, Melville, NY 11747. We serve patients from Melville NY, Brentwood NY, Farmingdale NY, Huntington NY, Commack NY, Lindenhurst NY.

Check Out Our 5 Star Reviews


Additional Services You May Like

Additional Services You May Like
- Abdominal Pain
- Acid Reflux
- Barretts Esophagus
- Bloating
- Capsule Endoscopy
- Celiac Disease
- Colon Cancer Screening
- Colonoscopy
- Constipation
- Crohns Disease
- Diarrhea
- Diverticulitis
- Esophageal PH Monitoring
- Fatty Liver
- Fibroscan
- Gallstones
- Gastroenterologist
- Gastric Chest Pain
- Gluten Intolerance
- Hemorrhoid
- Hemorrhoid Banding
- Hepatitis
- Irritable Bowel Syndrome
- Lactose Intolerance
- Pancreatitis
- Polyps
- Rectal Bleeding
- Stomach
- Ulcerative Colitis
- GI Urgent Care





